Ending the global health delivery gap
About 4.6 billion people lack essential health care. Not for lack of medical knowledge, but because health systems struggle to integrate what works and deliver it reliably.
We close this gap by delivering population-based comprehensive primary health care in underserved communities, and building from that work the computational architecture that makes it possible at scale.
Up to 90% of people's health needs can be addressed close to home — prevention, screening, treatment of common conditions, the management of chronic disease over time. Primary health care is how good population health is built, and where the largest gains for the world's poorest communities can be made.
Primary health care as the foundation
The hardest problem in global health is not making something work once, but making it work the same way the thousandth time. Pilots can demonstrate possibility; only replicable models change reality. We design every part of how we deliver care — protocols, care pathways, tools — to work the same in places far from where we first built them.
Design for scale
Comprehensive care for populations means coordinating thousands of actions across homes, clinics, and providers over time. This cannot be done manually, and existing digital tools address only parts of the problem. A computational architecture is needed to make integrated, population-based care operationally tractable — a Primary Health Care Operating System.
Develop the operating architecture
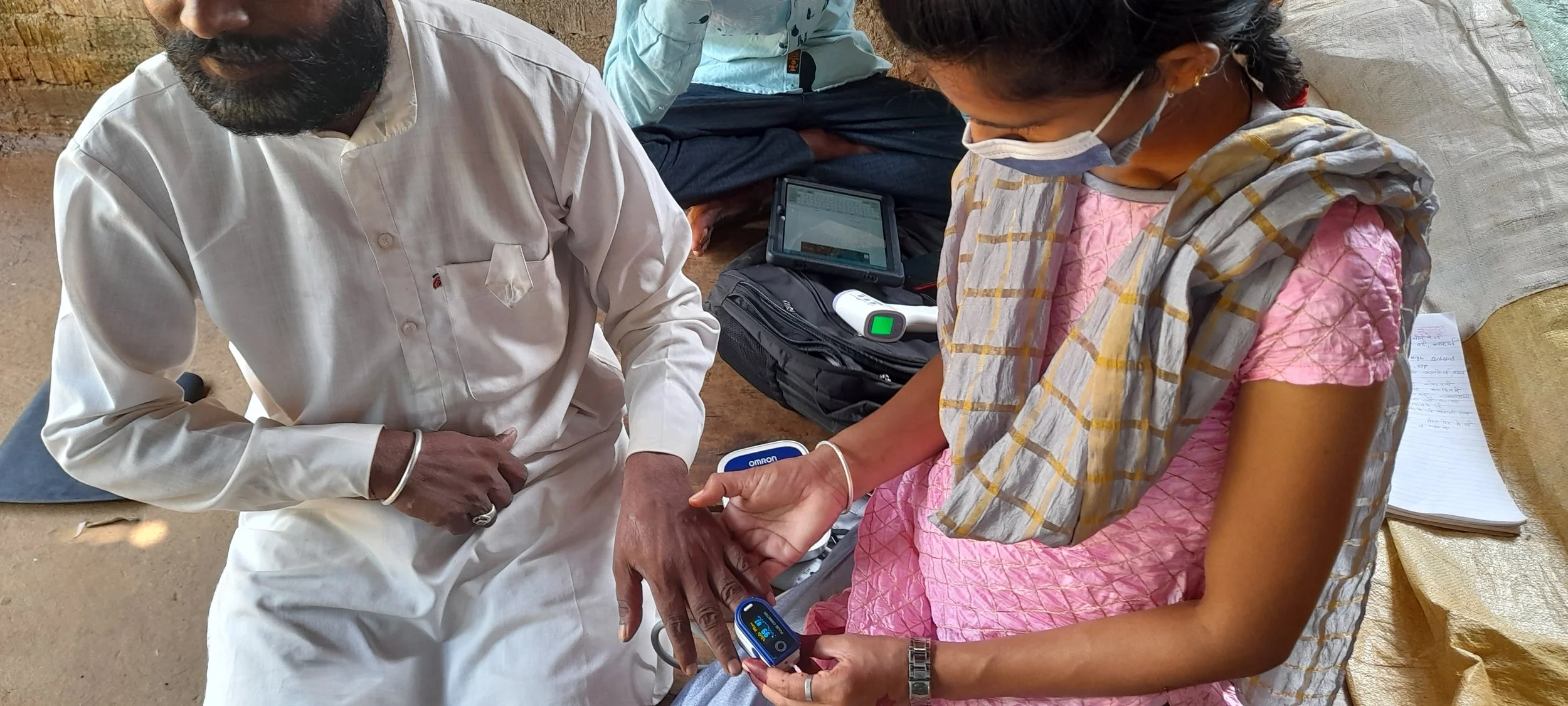
Optimize Health delivers primary health care in rural communities in Madhya Pradesh, India. Our teams provide comprehensive care to the families and villages we serve — managing chronic disease, screening for risk, addressing acute illness, and following individuals over time.
Where we work